“For me, a child is a blessing,” says Abigail Hendricks, who benefited from a brand new drug trial for preeclampsia. Right here she is together with her virtually 9-month-old, Hayden
Tommy Trenchard for NPR
disguise caption
toggle caption
Tommy Trenchard for NPR
It was the autumn of 2024 when Abigail Hendricks realized she was pregnant together with her fifth little one. She was glowing with pleasure.
“For me, a child is a blessing,” says Hendricks. “They’re cute. They’re valuable. And they’re a present from God.”
However Hendricks, who was 33 on the time and residing in Cape City, South Africa, would later be taught that her rising child was additionally a grave well being threat to her. Hendricks already had hypertension. Quickly, the complications started. Infrequently, her imaginative and prescient would blur. Then protein began exhibiting up in her urine.
“I stored on combating,” she recollects. “I did go to church. I pray within the morning. I pray at evening for my child to be secure and for me to be secure.”
Her medical doctors put her on a unique blood strain medicine and advised her to relaxation. By this time, all of Hendricks’ appointments had shifted to Tygerberg hospital, a facility in Cape City outfitted to deal with extra advanced circumstances.
However a month earlier than she was as a result of give start, she was dropping blood strain management. A traditional studying is 120 over 80, however hers climbed to 163 over 101.
Hendricks had developed preeclampsia, a probably deadly complication of being pregnant involving injury to the blood vessels and excessive quantities of fluid loss. It might probably result in harmful swelling of the lungs, mind, and coronary heart and large hemorrhaging.
“They advised me I can have a seizure as a result of the blood strain is simply too excessive,” she says. “It made me really feel scared and anxious. Like, what’s going to occur now?” (Eclampsia refers back to the seizures that happen in pregnant girls with preeclampsia.)
The medical staff believed Hendricks’ life was at risk — and so was her child’s.
An anxious starting

Cathy Cluver, professor of obstetrics and gynecology on the College of Stellenbosch (proper), embraces a pregnant mom at Tygerberg Hospital in Cape City. “Your child’s very excited to come back and meet you,” she tells her. Cluver, leads a analysis staff conducting a trial for a brand new drug to deal with preeclampsia, a probably harmful situation throughout being pregnant.
Tommy Trenchard for NPR
disguise caption
toggle caption
Tommy Trenchard for NPR
On a latest morning, Cathy Cluver glides by means of the bustling maternity ward of Tygerberg Hospital. Provide carts are wheeled down the hallway. Nurses and medical doctors transfer between their many sufferers. A new child child’s first cry pierces the air. Cluver is a professor of obstetrics and gynecology at close by Stellenbosch College, and he or she’s been trying to find a therapy for preeclampsia for a decade.
“We do about eight to 9,000 deliveries right here a 12 months of solely high-risk girls,” explains Cluver, together with these with preeclampsia who do their finest to delay supply. It is necessary for a child to remain contained in the womb so long as doable however this could jeopardize the well being of the mom.
Cluver factors to a room containing moms with preeclampsia. “You’ll be able to see they don’t seem to be trying nicely,” she says. “Their ft and their legs are swollen, and their arms are swollen. These mums are placing their very own lives in danger for the sake of the newborn.”
Preeclampsia happens when the placenta sends out a form of molecular misery name that it is not getting sufficient oxygen. “It is saying, ‘I want extra blood provide, so I am going to push the blood strain up,'” says Cluver, who had preeclampsia herself when she was pregnant together with her first little one.
Standard drugs to deal with hypertension are dangerous as a result of though they could decrease the mom’s blood strain, they might additionally cut back blood circulation to the newborn — proper when the placenta is demanding extra oxygen.
“It actually is likely one of the most severe issues of being pregnant,” says Cluver, making it one of many main causes of maternal mortality worldwide — with a minimum of 42,000 maternal deaths every year.
Cluver has been trying to find a therapy that lowers blood strain and heals the broken blood vessels to assist each mom and child. Then, about two years in the past, she acquired an electronic mail from DiaMedica Therapeutics, a U.S.-based pharmaceutical firm.
They had been testing a drug for sure forms of stroke known as DM199 that functioned in a manner they thought may additionally work for preeclampsia. Cluver was skeptical at first, however on nearer inspection, she and her colleagues thought possibly it was price attempting out. “It may probably work as a result of it is ticking all of the containers of what we’d need,” she says.
So that they started a trial on the hospital for moms with dangerously hypertension and who had been scheduled to ship their infants early.
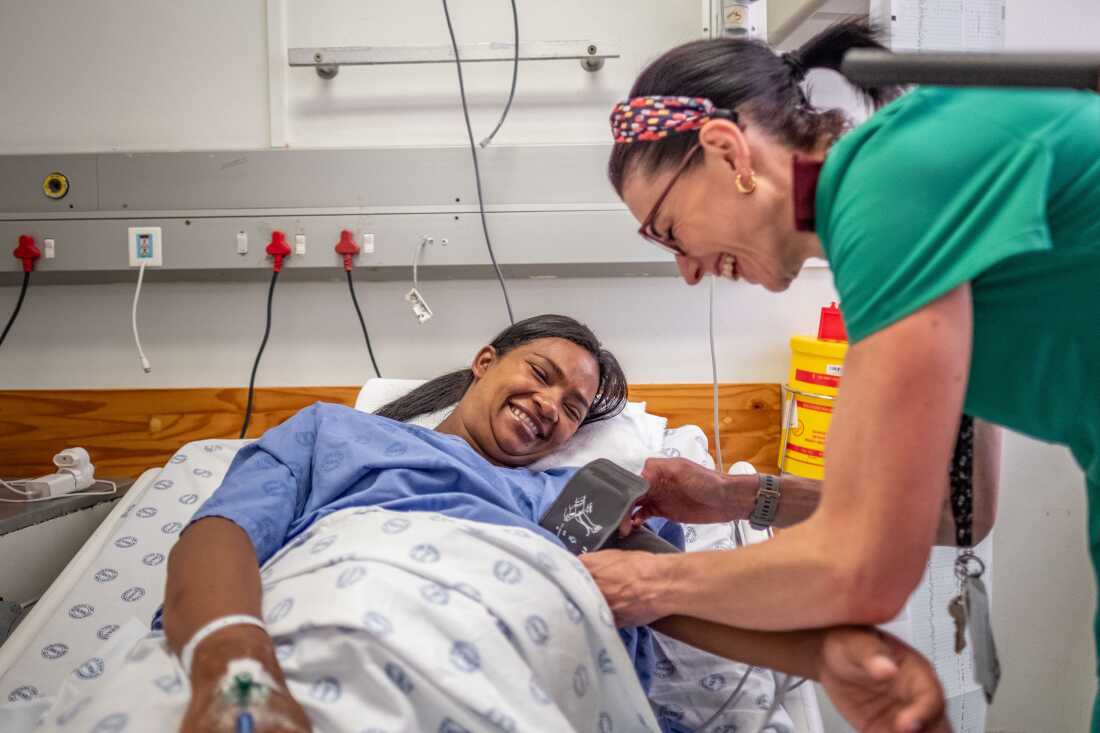
Jacqui Thake, a analysis nurse at Stellenbosch College who’s overseeing the drug trial, measures the blood strain of one of many sufferers on the hospital.
Tommy Trenchard for NPR
disguise caption
toggle caption
Tommy Trenchard for NPR
“I used to be so nervous that first day,” says Cluver. “We began the infusion and also you by no means fairly know what is going on to occur.”
The staff enrolled small teams of girls with every group receiving a barely increased quantity of the drug. Fifteen sufferers in, there was no signal that it was having any impact.
“I believed, ‘this drug isn’t actual,'” says Jacqui Thake, a analysis nurse at Stellenbosch College who’s overseeing the trial. “There was actually no distinction within the blood strain — possibly barely right here and there however nothing main.”
Fortunate quantity 16
When the sixteenth affected person obtained the subsequent highest dose, nonetheless, “we actually simply opened up this IV infusion after which her blood strain stabilized,” recollects Cluver. “We instantly noticed these sky-high blood pressures coming down and we had been like, ‘We do not consider this. That is inconceivable!'”
“That is truly when the actual pleasure began,” says Thake. “Like leaping up and down. I [sent] a gazillion emojis celebrating the blood strain happening.”
And it stayed down. The identical was true for subsequent sufferers with the identical or incrementally increased doses.

The drug trial requires the common sampling of the blood of individuals. Right here, analysis nurse Jacqui Thake pulls out a handful of these samples from one of many -80°F freezers.
Tommy Trenchard for NPR
disguise caption
toggle caption
Tommy Trenchard for NPR
“The drug stabilizes the liner of the blood vessels so it makes the blood vessels happier,” says Cluver.
Exams present the drug would not seem to cross into the placenta or the breastmilk both, which implies it is possible not reaching the newborn.
Cluver and her colleagues are hopeful that this could be the primary pharmaceutical therapy for preeclampsia.
“It could imply a wholesome mother and a wholesome child,” says Thake, who talks about what it could be wish to lose a mom or little one. “It could imply much less damaged houses and probably a greater life for the little ones rising up. That is what it might imply to me — a mother and a child rising up with love.”
Nonetheless, she says there’s extra to find out about how the drug works and whether or not it may preserve moms pregnant for longer.

This frozen vial accommodates DM199, a brand new experimental drug that researchers hope could be the first pharmaceutical remedy for preeclampsia.
Tommy Trenchard for NPR
disguise caption
toggle caption
Tommy Trenchard for NPR
Corneila Graves is the medical director of Tennessee Maternal Fetal Drugs, a facility the place she says as much as 10% of pregnant girls have preeclampsia.
“This can be a small research — it has nice potential however we want an even bigger information set on a broader inhabitants,” says Graves, who isn’t concerned within the trial.
“However what is de facto promising about this specific research is that it additionally will increase placental blood circulation,” she provides. That’s, this new drug lowers the mom’s blood strain whereas additionally bettering blood circulation to the womb at a time when the newborn seems to want it.
Kara Rood, a maternal fetal medication doctor on the Ohio State College who is not contributing to the trial, feels equally inspired by the early outcomes. However she’s desperate to see how the drug impacts girls earlier of their pregnancies and never within the pressing moments proper earlier than their supply.
“I feel the actual take a look at can be whether or not this medicine can safely extend the being pregnant to lower these dangers and in the end enhance neonatal outcomes,” says Rood.

Analysis nurse Jacqui Thake walks alongside Abigail Hendricks and her child boy. When Hendricks turned affected person quantity 24 within the drug trial, the 2 girls fashioned a particular bond.
disguise caption
toggle caption
As for Abigail Hendricks, she was affected person quantity 24 within the trial at Tygerberg hospital. Her child son is nearly 9 months now. “Hayden is a candy little boy. He is very playful.”
Again when her blood strain stored going up final 12 months a number of weeks earlier than her due date, she enrolled within the trial and obtained the brand new drug simply earlier than the medical staff induced her. Hendricks’ blood strain slowly dropped.
After which, “he was delivered screaming,” she says. “Once I held my child for the primary time, I cried. I had a lot pleasure in my coronary heart to know that he’s alright. And I used to be alright.”
This story was supported by a grant from the Pulitzer Heart.

